Medical Image of the Week: Malignant Spinal Cord Compression
 Wednesday, February 10, 2016 at 8:00AM
Wednesday, February 10, 2016 at 8:00AM 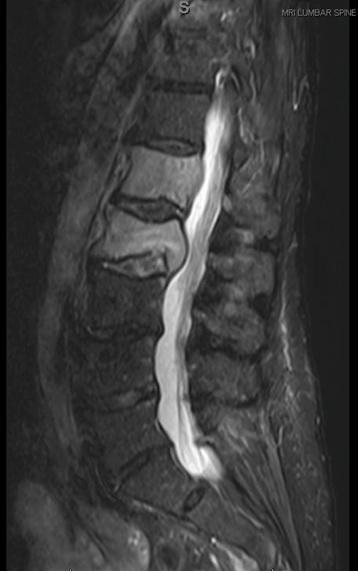
Figure 1. MRI lumbar spine (sagittal image) demonstrating increased signal in the L1 and L2 vertebral bodies with tumor erosion of the posterior cortices. Encroachment upon the spinal canal is noted at L2.

Figure 2. MRI lumbar spine (sagittal image, post gadolinium infusion) demonstrating heterogeneous enhancement of L1 and L2 consistent with metastatic disease; spinal cord compression is noted at L2 (blue arrows).
An 81 year-old man with metastatic bladder cancer was admitted to the hospital with back pain. The pain progressed over several weeks and interfered with ambulation. He had severe pain with any movement. Physical exam revealed pain with palpation of the lower back but no weakness or sensory deficits in the lower extremities. An MRI of the lumbar spine (with and without gadolinium contrast) revealed metastatic disease involving the L1 and L2 vertebral bodies, right sacrum and left iliac wing. At L2, moderate spinal canal stenosis due to tumor encroachment was noted (Figures 1 and 2). The patient was urgently treated with IV dexamethasone. He declined surgical intervention but agreed to radiation therapy.
Malignant spinal cord compression (MSCC) is an oncologic emergency that affects approximately 5% of cancer patients. It is most commonly seen in lung, breast, and prostate cancers (1). Neurologic complications are relatively uncommon in patients with bladder cancer. In a review of 359 patients with bladder cancer, only 2% had metastatic spinal cord compression (2). In MSCC, patients most commonly present with back pain. Weakness, sensory deficits, ataxia, paralysis, bowel and bladder dysfunction are later symptoms. The devastating effects of MSCC for patients make it imperative that clinicians consider the diagnosis in an oncology patient with back pain. The description of back pain can be vague and clinicians may overlook the insidious progression of symptoms. A crucial point related to the return of neurologic function in MSCC is the pretreatment neurological status. If treatment is started promptly, before significant weakness or other neurologic deficits develop, outcomes are notably improved. MRI of the total spine should be performed in any patient suspected of having MSCC. If MRI cannot be performed, CT with myelography is an alternative (3).
Treatment for MSCC includes steroids, radiotherapy, and surgery. The steroid doses vary widely and high dose steroids (dexamethasone 96 mg IV bolus with 24 mg four times daily for three days and taper over 10 days) are often initiated in patients with severe neurologic deficits. Lower dose steroids (dexamethasone 10 mg IV bolus, followed by 16 mg daily in divided doses) are also effective but there are no randomized controlled trials to compare efficacy of different doses. Radiation therapy is an important component of MSCC management, particularly in patients who are not surgical candidates. Both single dose radiation and longer course radiation have shown benefit, so decisions about dosing and duration can be based on the patient’s expected survival. Surgical decompression in addition to radiation therapy may provide quality of life benefits to a cohort of patients with MSCC. This avenue is reserved for patients with reasonable functional status and prognosis. A widely cited study published in 2005 showed improved functional outcomes after decompression plus radiotherapy versus radiotherapy only (4). If surgical intervention is considered, emergent consultation is critical to ensure the best possible outcome.
Katie Hawbaker MD, Michael Debo DO and Linda Snyder MD
Division of General Internal Medicine, Geriatrics and Palliative Medicine and Pulmonary, Allergy, Critical Care, & Sleep Medicine
Banner University Medical Center-Tucson
References
- McCurdy M, Shanholtz C. Oncologic emergencies. Crit Care Med. 2012;40:2212-2. [CrossRef] [PubMed]
- Anderson TS, Regine WF, Kryscio R, Patchell RA. Neurologic complications of bladder carcinoma. Cancer. 2003;97(9):2267-72. [CrossRef] [PubMed]
- Carter BW, Erasmus JJ. Acute thoracic findings in oncologic patients. J Thorac Imaging. 2015;30:233-46. [CrossRef] [PubMed]
- Patchell RA, Tibbs PA, Regine WF, Payne R, Saris S, Kryscio RJ, Mohiuddin M, Young B. Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: a randomized trial. Lancet. 2005; 366(9486):643-8. [CrossRef] [PubMed]
Cite as: Hawbaker K, Debo M, Snyder L. Medical image of the week: malignant spinal cord compression. Southwest J Pulm Crit Care. 2016;12(2):59-61. doi: http://dx.doi.org/10.13175/swjpcc160-15 PDF

Reader Comments