March 2015 Critical Care Case of the Month: It’s Not Always Sepsis
 Monday, March 2, 2015 at 8:00AM
Monday, March 2, 2015 at 8:00AM Dionne Morgan, MD
Carolyn H. Welsh, MD
University of Colorado and the Eastern Colorado Veterans Affairs Medical Center
Department of Medicine
Division of Pulmonary Sciences and Critical Care Medicine
Denver, CO
History of Present Illness
A 57-year-old man with multiple co-morbidities including diabetes mellitus presented with wet gangrene of the right foot and hypotension. He had diabetic ketoacidosis and acute kidney injury. He was admitted to the medical intensive care unit, given intravenous fluids and treated with insulin therapy, piperacillin/tazobactam and vancomycin. Initial blood cultures grew Methicillin-resistant Staphylococcus aureus (MRSA). The podiatry service performed a right transmetatarsal amputation. Subsequently, he did well and was transferred to a medical floor for further care.
Three weeks later, following resolution of the initial sepsis, he developed persistently high fevers with hemodynamic instability despite continued antibiotic therapy. He was transferred back to the MICU for presumed sepsis.
Past Medical History, Social History and Family History
The past medical history was significant for diabetes, hypertension, COPD, coronary artery disease and hepatitis C. He did not smoke nor drink alcohol. Family history was non-contributory.
Physical Examination
On readmission to the medical intensive care unit, the patient was noted to have a generalized maculopapular rash on both upper and lower extremities, torso, palms and soles of his feet, associated with facial and periorbital edema (Figure 1). There was no mucosal membrane involvement or lymphadenopathy. He was also febrile to 104o F, hypotensive to 80/50 mm Hg and icteric.
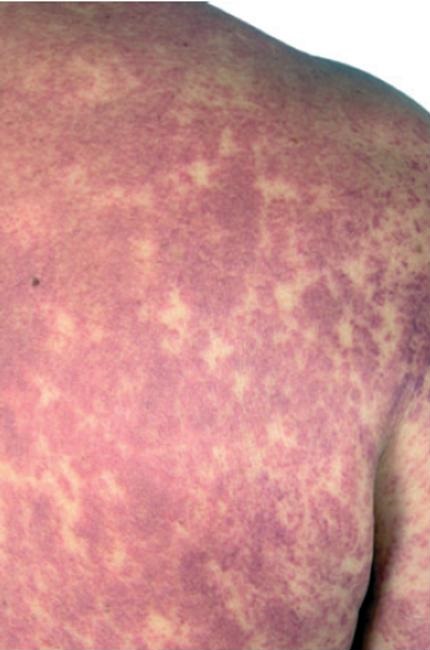
Figure 1. Image of rash.
Laboratory Studies
Initial labs showed elevated leukocyte count, BUN and creatinine with anion-gap metabolic acidosis but a normal liver enzyme profile. Repeat labs on readmission to the medical ICU were significant for severe leukocytosis, with marked eosinophilia, atypical lymphocytes on blood smear, acute transaminitis and hyperbilirubinemia.
Admission labs: White blood cell count (WBC) 29.9 x 1000 cells/μL. Eosinophils 0.0% (Normal 0.0 - 0.7%), AST 28 U/L, ALT 15 U/L, ALP 162 U/L, total bilirubin 0.2 mg/dL.
Labs on ICU readmission: White blood cell count (WBC) 35.7 x 1000 cells/ μL. Eosinophils 2.3% (Normal 0.0 -0.7%), AST 486 U/L, ALT 288 U/L, ALP 749 U/L, total bilirubin 4.3 mg/dL.
Which are components of the SIRS criteria? (click on the correct answer to proceed to the second of 4 panels)
Reference as: Morgan D, Welsh CH. March 2015 critical care case of the month: it's not always sepsis. Southwest J Pulm Crit Care. 2015;10(3):105-11. doi: http://dx.doi.org/10.13175/swjpcc029-15 PDF

Reader Comments